An EMR dashboard is not just a reporting screen. It is a decision system that helps clinical leaders, practice managers, and operations teams see what needs attention now: where patient flow is slowing, which tasks are overdue, what revenue is getting stuck, and which quality measures are drifting off target.
For most healthcare organizations, the pain is familiar. Teams are working inside the EMR all day, yet critical signals remain buried across appointment schedules, charting workflows, task queues, billing modules, and patient communication tools. By the time someone identifies a delay, the operational cost is already real: longer waits, incomplete documentation, missed follow-up, denied claims, and avoidable staff overload.
A well-built EMR dashboard solves that problem by turning raw records into a small set of high-value signals that support faster action.
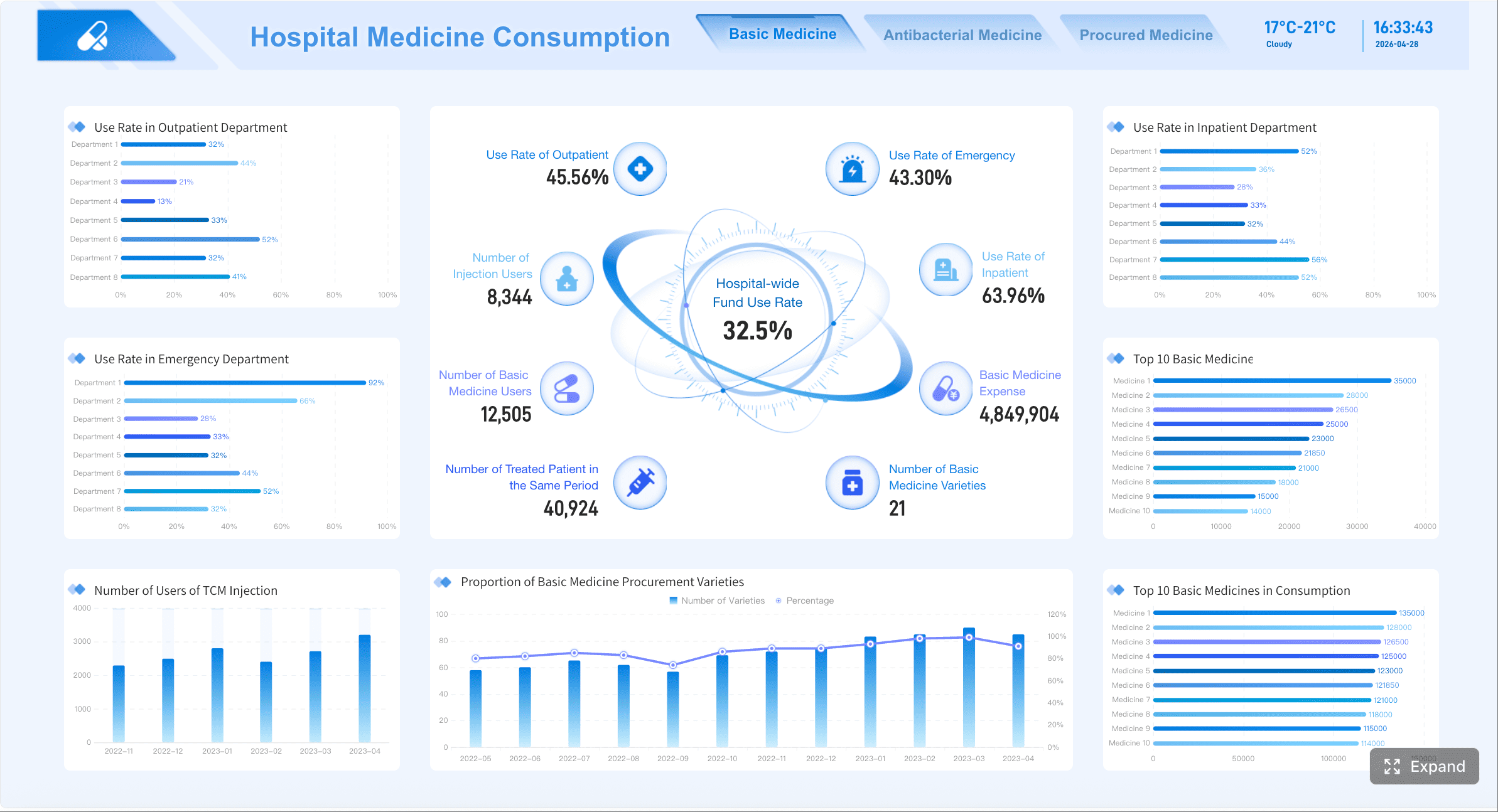
All dashboards in this article are created by FineBI
An effective emr dashboard gives decision-makers a real-time or near-real-time view of performance across care delivery, operations, and revenue workflows. Instead of forcing users to pull multiple reports, it consolidates the metrics that directly influence daily decisions.
At a glance, teams should be able to answer questions like:
That is the business value. Better visibility drives faster intervention, and faster intervention improves patient experience, staff efficiency, compliance, and financial performance.
A strong dashboard also changes the nature of EMR data. Raw records are detailed but fragmented. A dashboard organizes those data points into trends, thresholds, and exceptions. That makes it easier to move from observation to action.
For example, a scheduler does not need a list of every appointment record. They need to see unused slots, no-show patterns, and provider utilization by day and hour. A clinical manager does not need every note timestamp. They need to know chart closure time, overdue documentation volume, and which providers or teams need support.
The difference between a general reporting view and a decision-focused performance view is simple:
Below are the core KPI categories most organizations should define before building an EMR dashboard:
The best emr dashboard does not try to display everything. It prioritizes the metrics that influence daily clinical and operational decisions. The 12 metrics below give most practices a practical, high-impact foundation.
Appointment volume shows demand. Scheduling utilization shows how effectively capacity is being used. Together, they reveal whether your practice has access constraints, underused provider time, or unstable booking patterns.
Track this by day, week, provider, specialty, and location. Look for open slots that consistently go unused, time windows with elevated no-show risk, and schedules that rely too heavily on overbooking.
Key indicators include:
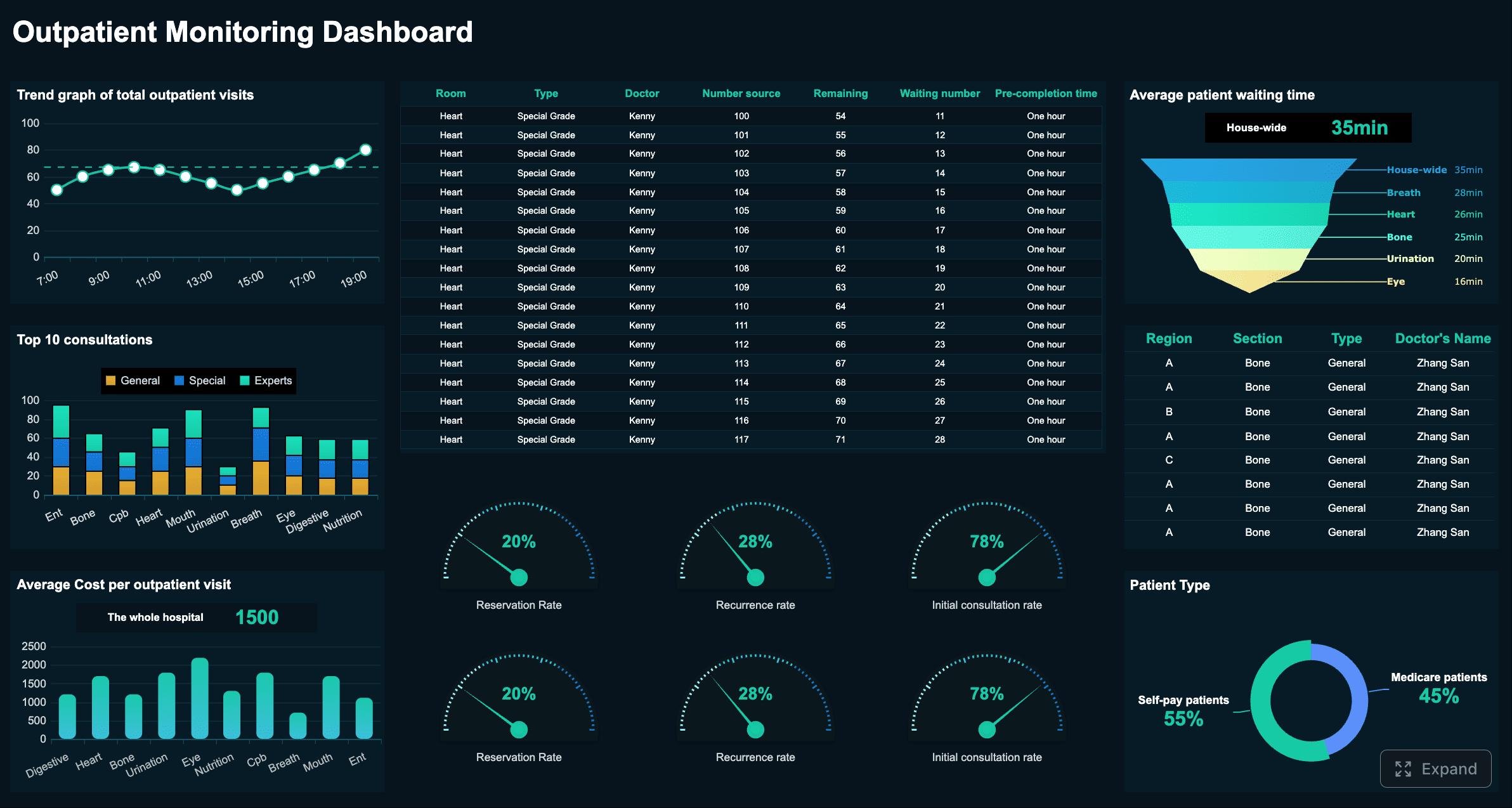 Outpatient Monitoring Dashboard created with FineBI
Outpatient Monitoring Dashboard created with FineBI
This metric is especially useful for access management, staffing, and template redesign.
Patient wait time is one of the clearest signals of operational friction. It affects patient satisfaction, clinic efficiency, and provider productivity.
A useful dashboard should break wait time into stages, not just one total number:
This lets managers see exactly where the bottleneck exists. Maybe front desk throughput is fine, but room turnover is slow. Maybe rooming happens quickly, but providers are routinely delayed by documentation spillover from earlier visits.
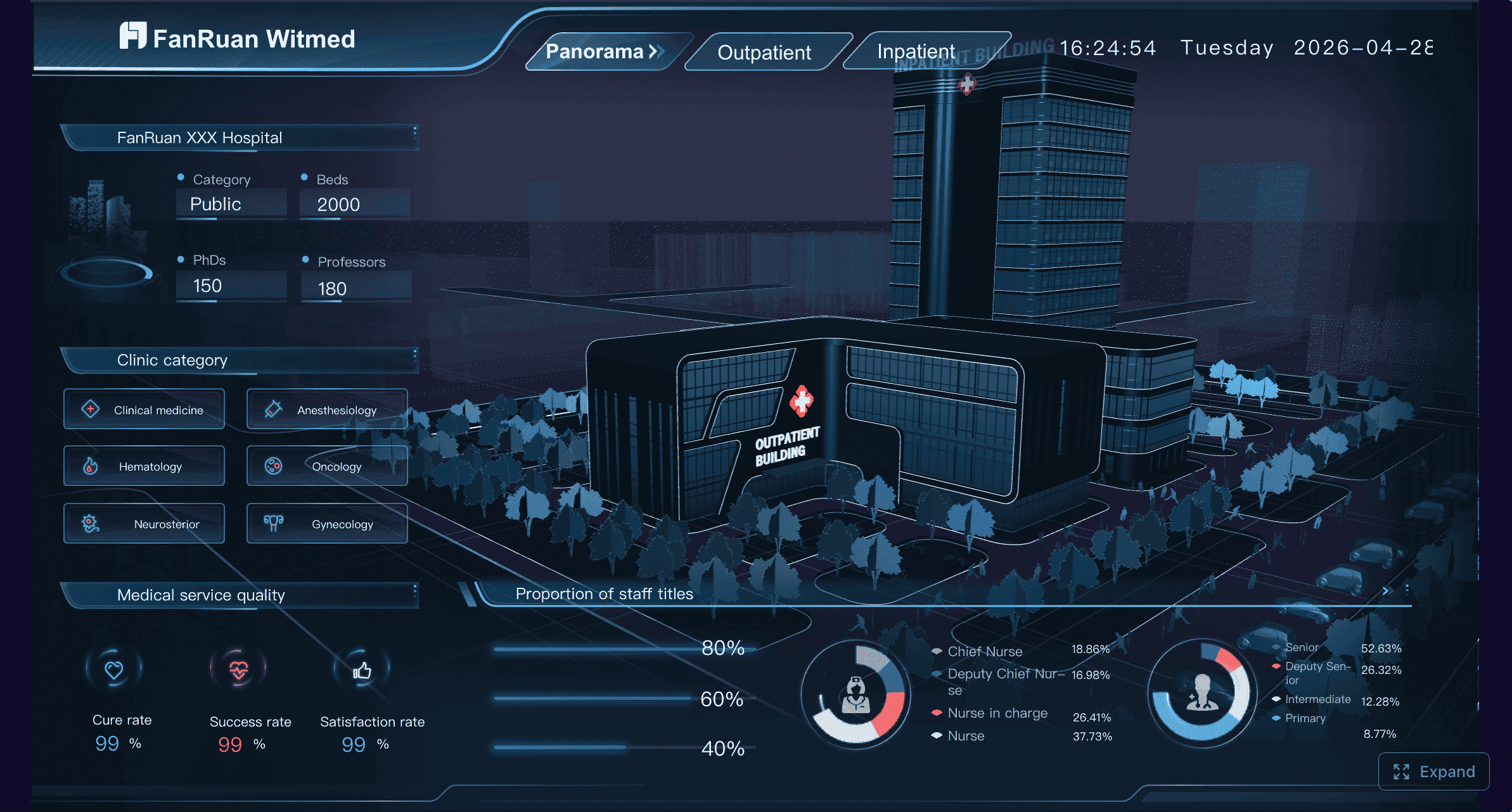 Hospital 360° Operations Dashboard created with FineBI
Hospital 360° Operations Dashboard created with FineBI
The goal is not simply to reduce averages. It is to identify variability, peak periods, and recurring failure points that disrupt care flow.
No-shows and cancellations directly affect access, revenue, provider utilization, and continuity of care. A dashboard should segment these rates by:
This level of detail helps teams move beyond generic assumptions. A spike in no-shows may be tied to one provider schedule, one specialty, or one appointment type. It may also reveal that reminder workflows are working for some patient groups but not others.
Operationally, this metric supports changes in reminder timing, waitlist activation, scheduling policy, and overbooking strategy.
Documentation lag creates downstream problems fast. Open charts delay coding, slow billing, weaken handoffs, and increase compliance risk.
An emr dashboard should show:
This metric helps leaders distinguish between isolated delays and structural workflow issues. If one department consistently closes notes later than others, the solution may involve template optimization, staffing support, or schedule redesign rather than simple performance pressure.
Clinical quality measures connect the EMR dashboard to patient outcomes and payer incentives. These metrics vary by organization, but common categories include:
The dashboard should focus on the measures that matter most operationally and financially. If teams are flooded with too many quality indicators, attention gets diluted. Instead, surface the measures tied to your current contracts, care priorities, and population health goals.
Make performance visible at both summary and drill-down levels. Leaders need trend lines and benchmark views. Care teams need patient-level follow-up lists tied to the same metrics.
Refill delays create patient dissatisfaction, staff burden, and potential clinical risk. They also consume significant inbox time for nurses, medical assistants, and providers.
Track:
This metric is valuable because it sits at the intersection of responsiveness and labor efficiency. If refill turnaround is slipping, the issue may be staffing, workflow design, protocol clarity, or message routing inside the EMR.
A dashboard makes that visible before the backlog becomes unmanageable.
Outstanding orders and unreviewed results are high-risk areas. A robust dashboard should help teams see whether orders are placed, completed, resulted, reviewed, and acted on in time.
Core measures include:
This is one of the most important safety-oriented components of an emr dashboard. It helps reduce the chance of missed follow-up, delayed outreach, or results sitting unattended in queues.
A referral is only valuable if it moves through the care journey successfully. Many organizations track referral placement but lack visibility into whether the patient actually schedules and completes the visit.
Your dashboard should measure:
This helps identify friction points such as poor handoff processes, network leakage, patient communication breakdowns, or insufficient referral coordination.
For multisite practices and health systems, referral completion is also a strong indicator of care continuity and downstream revenue capture.
Clinical performance and financial performance are tightly connected. If encounter documentation, coding, or claim submission stalls, cash flow slows.
Track these timing metrics carefully:
This metric is especially important for practice administrators and revenue cycle leaders because it reveals whether revenue delays are caused upstream in clinical workflows or downstream in billing operations.
A good dashboard does not only show lag. It shows where lag starts.
Denials generate avoidable cost, consume staff time, and often signal process inconsistency. Your dashboard should break denials down by:
Also track rework volume, because denial rate alone does not show the labor burden created after the denial occurs.
The most actionable measures include:
Portal adoption influences access, communication efficiency, administrative workload, and patient convenience. It can reduce manual calls and paperwork when managed well.
Track portal metrics such as:
This data helps practices understand whether digital engagement is actually reducing workload or just shifting it. For example, rising portal messages with slow response times may indicate a staffing or triage issue rather than a success story.
For leaders, portal engagement is also a useful proxy for digital maturity and patient service accessibility.
Most EMR environments generate a constant flow of work: inbox messages, refill requests, chart tasks, order follow-up, claims edits, and patient communications. Without visibility, bottlenecks grow silently.
A strong dashboard should show:
This metric matters because overloaded teams make slower decisions. When work is unevenly distributed, patient service declines and burnout risk rises. A dashboard gives managers the information needed to rebalance work before delays spread across clinical and administrative operations.
Not every organization needs the same dashboard. The right emr dashboard aligns metrics to actual decisions, not generic reporting habits.
Start with the decisions your teams make most often.
A useful rule: if a metric does not lead to a clear action, it probably does not belong on the main dashboard.
Choose metrics that answer questions like:
Dashboards fail when users do not trust the numbers. That usually happens because field definitions are inconsistent, refresh timing is unclear, or calculations change over time.
To keep data trustworthy:
If one clinic defines “visit completed” differently from another, cross-site benchmarking becomes unreliable. Standardization is not optional.
Many dashboards underperform because they try to show too much at once. Users do not need every metric on the landing page. They need a compact summary of what matters most, with the ability to drill down when necessary.
Best practice:
Simplicity increases adoption. Clutter kills it.
A technically correct dashboard can still fail if it is slow, confusing, or irrelevant to the people expected to use it.
Healthcare teams do not have time to interpret vague visuals. The dashboard should be understood in seconds.
Use:
The most effective dashboards emphasize outliers and changes that require attention. Users should instantly recognize what is on track, what is slipping, and what needs intervention now.
Different roles need different views from the same data.
Do not force everyone into one universal dashboard. Relevance drives adoption.
A role-based design also reduces noise. Users see only the metrics they can influence, which increases accountability and speed.
Not every metric requires constant refresh. But some absolutely do.
Use higher refresh frequency for:
Use daily, weekly, or monthly refresh cycles for:
This balance improves usability and infrastructure efficiency while preserving decision value.
Even well-funded dashboard projects can underdeliver if the design ignores operational reality. The most common mistakes include:
Tracking too many vanity metrics without clear action paths
If nobody knows what to do when a metric changes, it should not occupy prime dashboard space.
Mixing inconsistent definitions across departments or locations
A metric that means different things to different teams creates confusion, not alignment.
Ignoring staff adoption, training, and workflow fit
Dashboards must fit how teams already work. If users need extra effort to interpret or access them, adoption drops fast.
Failing to validate dashboard outputs against source records and reports
One trust-breaking discrepancy can cause teams to abandon the dashboard entirely.
Designing for reporting instead of intervention
The goal is not to admire trends. The goal is to trigger faster decisions.
A dashboard creates value only when it changes behavior. To move from visibility to action, organizations should define a clear operating model around each core metric.
Each metric should have:
For example, if chart closure exceeds a defined time limit or if unreviewed lab results exceed a safe threshold, the responsible team should know exactly what happens next.
Every metric needs an owner. Not just someone who watches it, but someone who is responsible for responding when performance changes.
Examples:
Ownership turns a dashboard from passive reporting into active management.
Different metrics need different review rhythms:
Cadence matters because delayed review weakens the value of visibility.
Practice goals, workflows, and patient needs change. Your dashboard should evolve with them.
Use monthly reviews to ask:
The best emr dashboard is not static. It matures with the organization.
Building this manually is complex; use FineBI to utilize ready-made templates and automate this entire workflow.
For healthcare organizations, the challenge is rarely a lack of data. The challenge is turning fragmented EMR, operational, and revenue signals into role-based dashboards that teams trust and use. That means connecting multiple data sources, standardizing KPI definitions, building drill-down logic, setting refresh schedules, and delivering views that match how leaders, managers, and frontline staff actually work.
FineBI helps simplify that process.
With FineBI, teams can:
That matters because speed to insight is now a competitive advantage. Practices and health systems cannot afford to wait on manual spreadsheet workflows or disconnected reports when care delivery, staffing pressure, and revenue performance are all moving in real time.
If your goal is faster clinical and operational decisions, the path is clear: define the right metrics, design for action, and avoid building the entire reporting stack from scratch. FineBI gives you a more scalable way to operationalize the dashboard strategy and turn EMR data into decisions teams can act on every day.
A useful EMR dashboard should combine clinical, operational, and revenue metrics in one view. Common examples include appointment volume, scheduling utilization, patient wait time, no-show rate, documentation lag, claims lag, and task backlog.
It helps teams spot bottlenecks by showing delays across check-in, rooming, clinician time, and checkout. With that visibility, managers can act faster to reduce wait times and smooth throughput.
The highest-value metrics are usually appointment utilization, patient wait time, no-shows and cancellations, chart closure time, overdue tasks, revenue cycle delays, and quality measure trends. The right mix depends on your workflow and decision needs.
For operational use, real-time or near-real-time updates are best because teams need to respond during the day. Some quality and financial metrics can also be reviewed daily or weekly depending on the process.
A standard report mainly summarizes what already happened, while an EMR dashboard highlights what needs attention now. Dashboards are built to support faster action with trends, thresholds, and exceptions.

The Author
Lewis Chou
Senior Data Analyst at FanRuan
Related Articles

What Is an Application Monitoring Dashboard? Beginner’s Guide to Metrics, Widgets, and Use Cases
An $1 is a single, actionable view of your app’s health, performance, availability, and user experience. For IT managers, operations leads, SREs, and developers, its business value is simple: it shortens the time between
Yida Yin
May 25, 2026

Dashboard Local Beginner Guide: CRM Features, Follow-Up Automation, and Real Use Cases
If you are exploring $1 for the first time, the main value is simple: it helps you stop losing track of people after meetings, referrals, networking events, and early sales conversations. For solo operators, small teams,
Yida Yin
May 25, 2026
React Dashboard Tutorial: Build a Real-Time KPI Workspace from a UI Template
A $1 is most valuable when it becomes a working command center, not just a pretty admin screen. In this tutorial, the scenario is straightforward: you need to deliver a real time KPI workspace for operators, managers, or
Yida Yin
May 21, 2026